Internal Medicine Billing Services in the USA: 2026 Revenue, Medicaid & Patient RCM Growth Guide
If you operate a medical clinic in the USA, manage a family medical center, or oversee a growing community medical center, your revenue doesn’t just depend on patient volume.
It depends on how well your internal medicine billing services handle:
- Medicaid billing
- Medicare Advantage plans
- US medical insurance providers
- Medication prior authorization
- Patient RCM workflows
- Medical billing data entry accuracy
Search trends show increasing demand for:
- Medical clinic near me
- Medical center USA
- Medical insurance companies
- Medicaid coverage information
But behind every search is one critical issue: reimbursement complexity.
Why Internal Medicine Billing Is More Complex in the USA
Internal medicine practices manage high-volume chronic conditions requiring ongoing medication management, including:
- ADHD medication
- Anxiety medication
- Depression medication
- High blood pressure medication
- Thyroid medication
- Migraine medication
- Bipolar medication
- Gout medication
- Acne medication
Each prescription may require:
- Prior authorization
- Insurance re-verification
- Step therapy documentation
- Formulary validation
According to the Centers for Medicare & Medicaid Services (CMS), reimbursement structures vary significantly between Medicaid, Medicare Advantage, and private insurance providers.
Outbound Authority Link: https://www.cms.gov
That means a general medical billing company may not fully understand internal medicine risk exposure.
The Hidden Revenue Leak: Weak Medical Billing Data Entry Process
Many US medical clinics believe coding causes denials. In reality, most denials begin at the billing data entry process.
Common breakdown points:
- Incorrect Medicaid eligibility verification
- Wrong medical terminology selection
- High deductible health plan miscalculation
- Missing modifiers
- Delayed charge capture
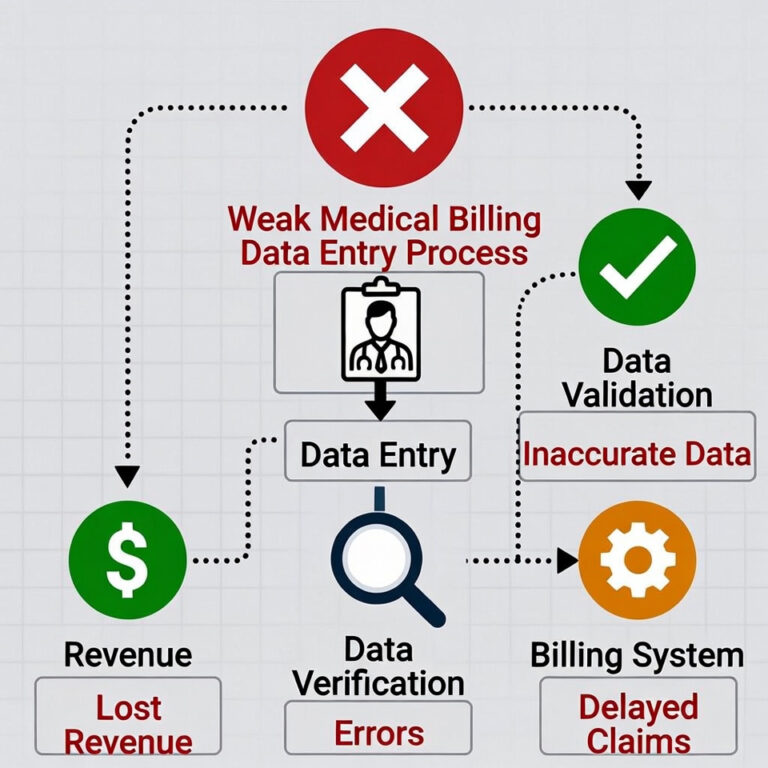
Even a certified medical assistant entering charges incorrectly can trigger claim rejection. Clinics now actively search for:
- Efficient medical data entry solutions
- Medical software companies
- Medical billing automation systems
Because automation reduces manual keystroke errors and improves clean claim rate.
Medicaid, Medicare Advantage & US Medical Insurance Complexity
American medical clinics must understand differences between:
- Medicaid USA programs
- Medicare Advantage plans
- Private health insurance companies
- Family health insurance policies
- Individual health plans
- High deductible health plans
Patients frequently ask:
- How much does medical insurance cost?
- How much is medical insurance per month?
- Is medical insurance tax deductible?
- How to apply for medical insurance?
- Does insurance cover medical marijuana?
When front desk teams cannot explain benefits clearly, patient collections decline.
For a full breakdown of payer complexity, see:
Medicaid, Medicare Advantage & Medical Insurance Billing Guide (Internal Link to Blog 3)
For official federal insurance marketplace guidance, visit:
Outbound Link: https://www.healthcare.gov
Medication Prior Authorization: The Largest Revenue Delay in Internal Medicine
Prior authorization delays for:
- ADHD medication
- Anxiety medication
- Thyroid medication
- High blood pressure medication
- Depression medication
can stall payments for weeks.
Structured authorization tracking improves turnaround time.
For full medication authorization workflow, see:
Medication Prior Authorization & Internal Medicine Billing (Internal Link to Blog 2)
Patient RCM in 2026: The Complete medical center USA Revenue Framework
Patient Revenue Cycle Management in the USA includes:
- Insurance eligibility verification
- Medicaid confirmation
- Copay and deductible education
- Claim submission
- Denial management
- AR follow-ups
- Payment posting
Modern internal medicine billing services integrate automation with human review.
The result:
✔ 95%+ clean claim rate
✔ Reduced AR days
✔ Higher net collection ratio
✔ Improved patient satisfaction
Outsourcing vs In-House Medical Billing in the USA
Average outsourced prior authorization support for a 5-provider US medical clinic:
- $1,200–$3,500 per month
OR - 4–8% of collections
Compare that to denial loss, which often exceeds 5–10% of revenue.
For professionals planning to build their own medical billing company, read:
Starting a Medical Billing Business in the USA (Internal Link to Blog 4)
Final Thoughts
Internal medicine billing services in the USA must connect:
Medicaid + Medicare Advantage + Medical Insurance + Medication + Patient RCM + Automation. Let Cureintent handle your billing because anything less results in revenue leakage.







