Prior Authorization Cost Guide: Pricing & Rates.
Before We Begin, A Quick Overview
In this guide, we’ll explore everything you need to know about prior authorization cost, including real USA pricing, hourly vs. monthly rates, budgeting tips, and how to get maximum ROI. This breakdown is written in a simple, friendly tone so you can understand costs without any confusion.
Understanding Prior Authorization Pricing in the USA
One of the most common questions healthcare practices and businesses ask is: “How much does a prior authorization cost?” The answer varies, but this guide will give you a clear and realistic picture of what to expect in 2025.
In the United States, prior authorization cost $10–50 per hour, depending on experience level, specialization, workflow complexity, and turnaround requirements. Compared to full-time in-house hires (which cost $50,000–$80,000 annually including benefits and overhead), outsourcing is significantly more affordable.
For many American practices, a prior authorization specialist working about 30 hours weekly may cost around $1,500/month. Hiring a full-time staff member for the same workload often costs $4,000–$6,000/month once salary, benefits, management, and software tools are included. The savings are substantial—especially for medical offices looking to streamline operations while reducing operational cost.
Prior Authorization Pricing Models Explained
Prior authorization support is priced using different models. Understanding each helps you choose what fits your practice best.
Hourly Pricing ($10–50/hour)
Best for variable workloads or new practices. You pay only for hours used, making it flexible and cost-efficient. Example: A Georgia clinic uses this model during insurance-heavy months.
Monthly Retainer ($500–$3,000/month)
Ideal for consistent weekly volume. You get a fixed number of hours at a discounted rate, creating predictable monthly budgeting.
Per-Task Pricing (Varies)
Useful for defined tasks such as follow-ups, eligibility checks, or one-time insurance verification workflows.
Full-Time Dedicated Support ($1,500–$3,500/month)
Perfect for high-volume practices needing 40+ hours weekly. You get a dedicated prior authorization expert who works like an in-house staff member but at a far lower cost.
Service Tier Comparison:
| Service Level | Hourly Rate | Monthly Package | Best For |
|---|---|---|---|
| Basic | $10–15/hr | $400–600 | Simple tasks, startups |
| Standard | $15–25/hr | $600–1,200 | Small practices |
| Professional | $25–40/hr | $1,200–2,000 | Growing clinics |
| Premium | $40–60/hr | $2,000–3,500 | Complex medical workflows |
Factors That Affect Prior Authorization Costs
Knowing what impacts pricing helps you make more informed decisions.
Experience Level
Entry-level: $10–18/hour
Mid-level: $18–30/hour
Senior specialists: $30–50/hour
The more experienced the specialist, the faster and more accurately they can handle insurance workflows.
Specialization
General support is cheaper. Specialized expertise (e.g., cardiology, radiology, behavioral health) costs more because accuracy requirements are higher.
Geographic Factors
USA-based specialists are pricier due to time alignment and compliance standards, but many practices prefer them for smoother coordination.
Hours & Commitment
Longer commitments receive discounted rates. A 40-hour/week plan may cost 15–20% less per hour compared to smaller plans.
Cost Comparison: Prior Authorization Specialist vs. Full-Time Employee
Let’s compare real annual costs:
Full-Time Employee (Annual)
• Salary: $40,000–55,000
• Insurance: $7,000–15,000
• Taxes: $3,500–5,000
• PTO: $3,000–4,000
• Equipment & Software: $2,000–3,000
• Office Space: $3,000–10,000
Total: $59,500–94,000/year

Prior Authorization Outsourcing (Annual)
• Monthly Cost: $1,500–2,500/month
• Total Annual: $18,000–30,500
Savings: $40,000–65,000/year
| Category | Full-Time Employee | Prior Authorization | Savings |
|---|---|---|---|
| Salary/Pay | $45,000 | $18,000 | $27,000 |
| Benefits | $12,000 | $0 | $12,000 |
| Overhead | $8,000 | $0 | $8,000 |
| TOTAL | $65,000 | $18,000 | $47,000 |
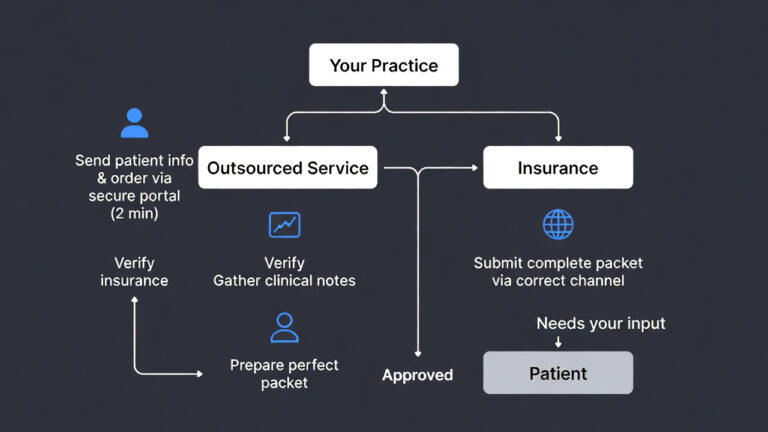
How to Make Prior Authorization Easier
Prior authorization feels complicated, but it becomes much simpler when you follow a clear process. A few small steps can speed up approvals, reduce mistakes, and lower your overall prior authorization cost. The goal is to keep everything organized and remove the manual stress from your team.
Simple ways to make PA easier:
• Keep all documents (insurance card, clinical notes, codes) ready before submitting
• Use a small checklist so every request is clean and complete
• Track each PA request to avoid delays or missed follow-ups
• Fix common denial reasons so the same mistakes don’t repeat
• Let trained PA specialists handle the busy work so your team can focus on patients
Conclusion
Understanding prior authorization cost helps you make better decisions for your practice. Outsourcing to a trusted partner like CureIntent can cut your expenses by 50–70%, speed up approvals, and free your team from stressful paperwork. It’s a simple way to keep your focus on patient care instead of admin tasks.
If you’re still figuring out What is Prior Authorization? or How to Get Started with Prior Authorization, start small. Try a basic package, track your results for 30 days, and increase hours as your practice grows. Even a small step can bring noticeable improvements. Learn more about the definition and purpose of prior authorization(click here)