How to Make Prior Authorizations Easier
In this guide, we’ll walk you through easy, clear, and stress-free ways in order to know how to make prior authorizations easier for your team and your patients, so your day feels lighter and your revenue stays on track.
Why Prior Authorizations Feel Hard
Many US healthcare practices struggle with PAs because of:
- Long phone calls
- Missing documents
- Wrong codes Tools That Make Prior Authorizations Easier
- Slow payer responses
- Busy staff
Everyone should know, How to Make Prior Authorizations Easier
These easy tips These easy tips work for clinics of every size, small offices, group practices, specialty centers, and multi‑location providers. That’s exactly how to make prior authorizations easier across different settings, ensuring smoother approvals and faster patient care for clinics of every size, small offices, group practices, specialty centers, and multi-location provider.
1. Always Check Eligibility First
This prevents last-minute surprises and rejected requests.
2. Keep All Patient Info Clean and Correct
Small data mistakes cause the biggest delays.
3. Use Clear CPT & ICD-10 Codes
Right codes = smooth approvals.
4. Create a PA Checklist for Your Staff
One checklist can save hours every week.
5. Track Every PA in One Place
Use a dashboard, spreadsheet, or practice management tool.
6. Set Daily Follow-Ups
Even 5-minute check-ins keep everything moving.
7. Outsource if PAs Take Too Much Time
Many US clinics now use outsourcing to get approvals faster and reduce costs.
Before vs. After: How PAs Improve with a Better System
| Problem Before | Better After |
|---|---|
| Slow approvals | Faster turnarounds |
| Missing documents | Organized checklists |
| Staff burnout | Light, easy workload |
| High denials | Cleaner submissions |
| Patient delays | Smooth scheduling |
| Unclear status | Full tracking and updates |
How Prior Authorization Outsourcing Helps (USA Market)
Many clinics in Texas, Florida, California, New York, Georgia, and Arizona outsource prior authorizations because:
- It costs less
- Approvals move quicker
- Staff get more time for patient care
- Experts know payer rules better
- Denials drop
- Cash flow improves
Even small clinics save 50–70% on time and cost.
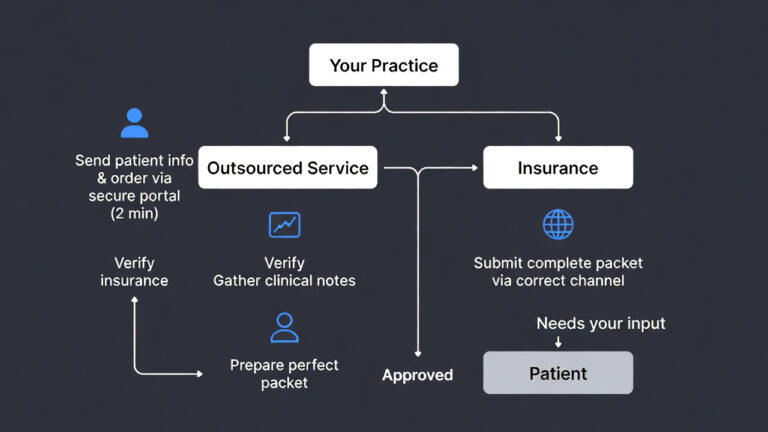
Quick Step-by-Step Guide to Make PAs Easier
Think of this as your simple tutor-style flow:
Step 1: Check Patient Eligibility
Confirm coverage, plan details, and payer rules.
Step 2: Gather All Documents in One File
Notes, reports, codes, and test results.
Step 3: Submit the PA Cleanly
Double-check everything.
Step 4: Track the Status Daily
A quick follow-up prevents long delays.
Step 5: Update the Patient
Patients feel relaxed when they know what’s happening.
Cost Comparison: In-House vs Outsourced Prior Auths (USA)
| Model | Average Monthly Cost | Best For |
|---|---|---|
| In-House Staff | $4,000 – $6,500 | Large practices who need full control |
| Outsourced Team | $900 – $2,500 | Clinics wanting faster, cheaper approvals |
| Hybrid Model | $1,500 – $3,000 | Growing practices needing flexible help |
Top States Searching for PA Help
These states show the highest search volume for prior authorization support:
- Texas
- Florida
- New York
- California
- Illinois
- Georgia
- Arizona
If your clinic is in any of these states, improving your PA workflow can boost speed and revenue.
Tools That Make Prior Authorizations Easier
You don’t need fancy software. Just tools like:
- Electronic health records
- PA portals from payers
- Simple shared spreadsheets
- Task tracking apps
- Outsourced PA team with 24/7 workflow
When Should a Practice Consider Outsourcing Prior Authorizations?
Choose outsourcing when:
- You have too many denials
- Your staff is overloaded
- Your approvals are slow
- Your front desk is dealing with too much paperwork
- Patients are waiting longer
- Your revenue cycle is getting stuck

Even a small package (10–20 hours/month) can fix the entire workflow.
Final Thoughts
Prior authorizations become much easier when your clinic uses clean data, good tracking, and a simple step-by-step system. Many US practices now partner with CureIntent to reduce workload and speed up approvals. If you’re exploring Prior Authorization Jobs, checking the Prior Authorization Cost Guide: Pricing & Rates, or want to learn What is Prior Authorization? or How to Get Started with Prior Authorization, even small improvements can make your workflow smoother. For official payer rules, visit the CMS Prior Authorization Resource (https://www.cms.gov).