Outsourced Prior Authorization Services
Okay, let’s talk real talk. You’re searching this because you’re probably drowning in prior auth paperwork right now. Maybe you’re a clinic manager in Ohio watching your nurses spend hours on hold with Anthem. Maybe you’re a dermatologist in Florida dealing with 30 different prior auth forms. Or maybe you’re just tired, really tired of the whole insurance game.
I get it. And I’m going to walk you through exactly what outsourced prior authorization services are, what they really cost, and whether they’re worth it for YOUR practice.
What Exactly Are Outsourced Prior Authorization Services?
Outsourced Prior Authorization Services are specialized companies that take over the burden of insurance pre‑approvals for medical practices. Instead of your staff spending hours on hold with insurers like Cigna or Aetna, trained experts handle the entire process.
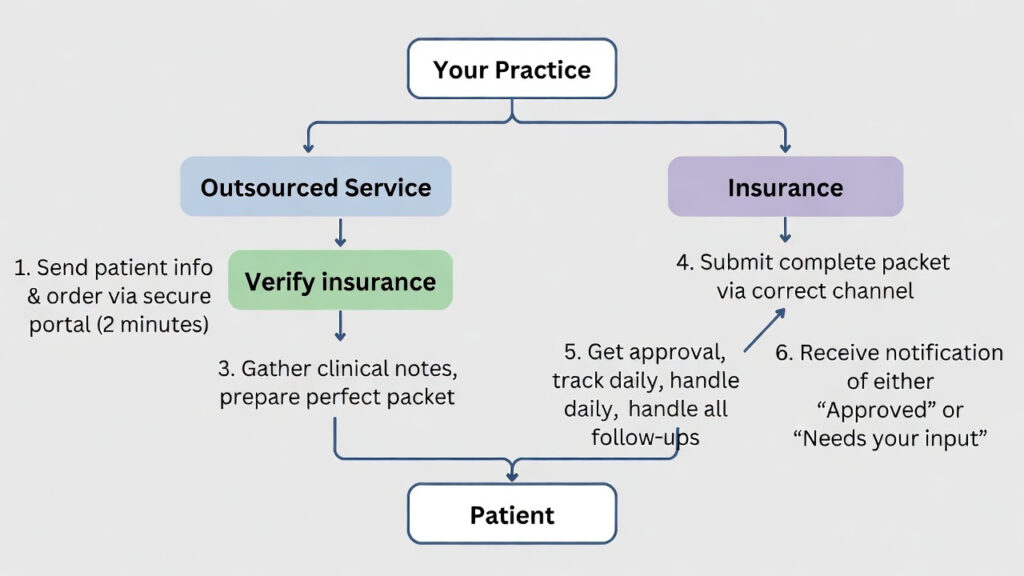
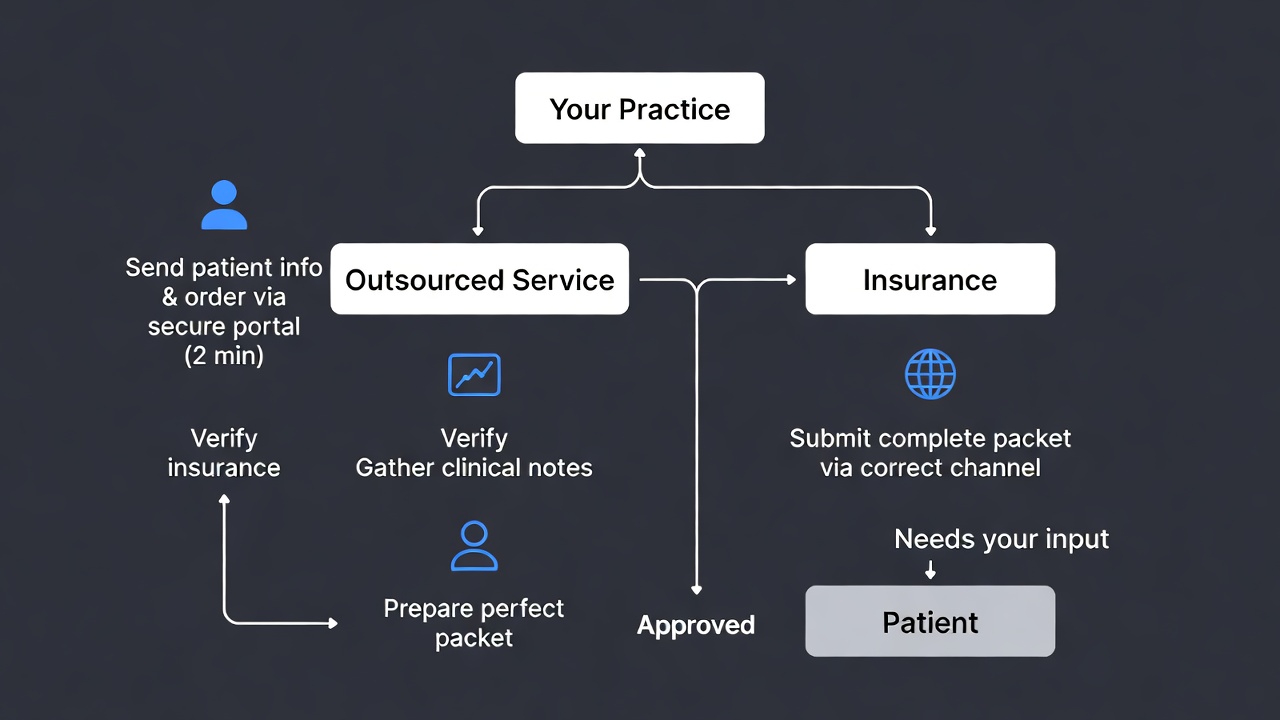
Notify your practice immediately when approvals are granted or if additional input is needed.
What they do:
- Collect patient information and clinical notes.
- Verify insurance coverage and requirements.
- Prepare and submit complete prior authorization packets.
- Track approvals daily and manage all follow-ups.
The Real Problem: Why Everyone’s Searching This Now
Let me show you what’s probably happening in your clinic right now:
Scenario 1: The Texas Cardiology Clinic
- Dr. Martinez’s nurse spends 3 hours daily on prior auths
- They perform 40 stress tests monthly
- 25% get denied initially
- Each appeal takes 2-3 days
- Result: Patients wait weeks, staff is burned out, money is left on the table
Scenario 2: The California Psychiatry Practice
- Therapist needs prior auth for every 8 therapy sessions
- Different rules for Medi-Cal vs Blue Cross
- Forms change quarterly
- Result: Constant training, constant errors, constant frustration
Scenario 3: The New York Physical Therapy Center
- 50+ patients weekly need authorizations
- Each takes 45 minutes to process
- That’s 40+ hours weekly just on paperwork
- Result: No time for actual patient care
Sound familiar? That’s why searches for “outsourced prior authorization solutions” are up 300% in the last year.
How It Actually Works: Step by Step
Here’s what happens when you work with a good service (we’ll talk about what “good” means in a minute):
Week 1: The Setup
You connect your system to theirs. This isn’t as scary as it sounds—most use secure portals that connect to your EHR. Think of it like adding a new app to your phone.
Week 2: The Handoff
Your staff stops filling out forms. Instead, they just:
- Click “Send to Auth Team”
- Attach the patient’s info
- Go back to patient care
Week 3: The Magic Happens
The service handles:
- Calling insurance companies (during THEIR business hours)
- Filling out each insurer’s specific forms
- Submitting through the right portals
- Tracking every submission
- Handling denials and appeals
Week 4: You Get Your Life Back
You get notifications like:
- “Mrs. Johnson’s MRI approved by UnitedHealthcare”
- “Need more info for Mr. Smith’s PT auth”
- “All 15 pending auths submitted and tracked”
What Does This Actually Cost in 2026?
This is what everyone really wants to know. Here’s the breakdown:
| Service Type | Typical Cost | Example | Best For |
|---|---|---|---|
| Per Auth | $18-$45 each | Arizona clinic: 40 auths × $28 = $1,120/month | Most clinics |
| Monthly Plan | $299-$1,500/month | Illinois practice: $899 for up to 50 auths | Steady volume |
| Hourly | $30-$70/hour | Solo practitioner: 10 hours × $45 = $450 | Testing phase |
| Bundled | 5-8% of collections | Florida surgery center: Included with billing | Growing practices |
Real Math Example:
A Michigan primary care clinic does 60 prior auths monthly:
- Current cost: 60 × 2 hours × $25/hour = $3,000 in staff time
- Plus: 12 denials × $250 in lost revenue = $3,000
- Total current cost: $6,000/month
- Outsourced cost: 60 × $30 = $1,800
- Monthly savings: $4,200
- Plus: Staff actually does medical work
The Good, The Bad, and The Ugly
The Good Parts:
- Time savings (obvious, but huge)
- Higher approval rates (experts know the tricks)
- Faster turnaround (patients get care sooner)
- Staff happiness (they went to school for healthcare, not paperwork)
The Bad Parts:
- Setup takes 2-4 weeks
- You need to learn a new system
- Some control feels “lost” (but isn’t really)
The Ugly Truth:
Some services are terrible. They outsource overseas, they don’t understand U.S. insurance, and they make more mistakes than they fix.
How to Pick a Good Service (Red Flags to Watch For)
🚩 Red Flag 1: No U.S.-based team
Why: Offshore teams don’t understand state-specific Medicaid rules or local insurance quirks.
🚩 Red Flag 2: Unclear pricing
Why: Hidden fees will destroy your savings.
🚩 Red Flag 3: No specialty experience
Why: Prior auths for rheumatology medications are different from orthopedic surgery.
🚩 Red Flag 4: Poor communication
Why: You need daily updates, not weekly reports.
🚩 Red Flag 5: No references
Why: If they won’t connect you with current clients, something’s wrong.
State-Specific Things to Know
For California Clinics:
Medi-Cal has different rules than commercial plans. Make sure your service knows both.
For Texas Practices:
Blue Cross Texas has different requirements than Blue Cross in other states.
For New York Providers:
Workers’ comp authorizations are a whole different ballgame.
For Florida Facilities:
Medicare Advantage plans each have their own forms and requirements.
What Your First Month Looks Like
Day 1-7: Setup and training. Your staff learns the new system.
Week 2: Start with 20-30% of your auths. See how it goes.
Week 3: Increase to 50-70%. Work out any kinks.
Week 4: Full transition. Your staff stops doing prior auths entirely.
The Bottom Line
Here’s the truth: If you’re spending more than $2,000 monthly on staff time for prior auths, outsourcing will save you money. Probably a lot of money.
But more importantly: What’s your staff’s time worth? What’s your sanity worth? What’s getting patients care FASTER worth?
The best clinics I’ve seen treat this like any other business decision: They calculate the ROI, they test it carefully, and if it works, they implement it fully. With Outsourced Prior Authorization Services, practices reduce costs and improve efficiency, and by relying on Outsourced Prior Authorization Services, they ensure patients get faster access to care.
Next Steps (If You’re Serious)
- Track your current time for one week. Be honest about every minute spent on prior auths.
- Calculate your current cost (staff time + denied claims + opportunity cost).
- Talk to 2-3 services. Ask for references from practices like yours.
- Start with a trial. Most good services will do 10-20 auths free or cheap to prove their value.
Final thought: The insurance companies have entire departments dedicated to making your life difficult. Maybe it’s time you had experts on YOUR side too. With Outsourced Prior Authorization Services, you gain a team that fights for faster approvals and fewer denials. Choosing Outsourced Prior Authorization Services means protecting your staff’s time, your revenue cycle, and your patients’ access to care.
Remember: Your job is patient care. Their job is paperwork. Let everyone do what they’re best at.