Prior Authorization Automation 2026: New Rules, AI Solutions & Case Studies
In this article, I’ve collected data from CMS, Gartner, and leading healthcare automation companies to create a full detailed guide on prior authorization automation in 2026. I’ve analyzed official press releases from R1 RCM, Optum, ZeOmega, Innovaccer, Infinx, and UiPath, plus real-world case studies from major health systems. Let me share everything I found.
What Is Prior Authorization Automation?
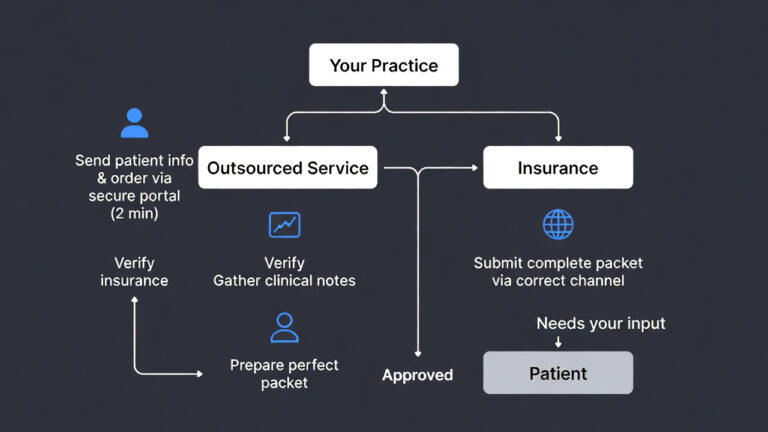
Prior authorization automation uses software robots and artificial intelligence to handle the insurance approval process automatically. Instead of your staff spending hours on phone calls and faxes, the computer does the work. It checks patient coverage, submits requests, tracks status, and handles denials. Your team only steps in for complex cases.
According to CMS data, prior authorization costs the healthcare industry an estimated $35 billion annually and causes 92% of care delays.
Official Statements from Leading Automation Companies
Here’s what the top automation software companies are saying about prior authorization in 2026.

R1 RCM
Website: www.r1rcm.com
Contact Name: Not specified (company press release)
Statement: On January 15, 2026, R1 RCM launched R1 Prior Authorization powered by the Phare Operating System. The company states: “Built on years of operational experience, R1 Prior Authorization is delivering measurable results for providers with 68% of all orders cleared in one hour and nearly 97% in one day, with an average auth-related denial rate of less than 1%.”
A Florida health system executive said: “Partnering with R1 to modernize prior authorization has transformed the speed at which we can move patients into care. Today, more than 99% of our prior authorizations are cleared within three days.”
Optum
Website: www.optum.com
Contact Name: Dr. John Kontor, M.D., Senior Vice President of Clinical Technology at Optum Insight
Statement: On February 4, 2026, Optum introduced AI-powered Digital Auth Complete. Dr. Kontor said: “We’re transforming the prior authorization process to address the friction it causes. By uniting clinical data, evidence-based criteria, and human-centered AI at every step, we’re making it simpler and faster for patients to get appropriate care.”
Optum’s solution eliminates 45% of manual touches and delivers an 80% increase in processing efficiency, with a 96% first-pass approval rate.
ZeOmega
Website: www.zeomega.com
Contact Name: Suhas Ramachandra, VP, Product Strategy and Innovation
Statement: ZeOmega was recognized in the 2026 Gartner Market Guide for Intelligent Prior Authorization. Suhas Ramachandra said: “As payers and providers face mounting financial and regulatory pressures, inefficiencies in prior authorization workflows amplify the strain. We believe ZeOmega’s recognition in this Gartner Market Guide reflects our continued commitment to helping healthcare organizations streamline prior authorization processes, improve efficiency and ultimately support faster access to care.”
Innovaccer
Website: www.innovaccer.com
Contact Name: Abhinav Shashank, Co-Founder and CEO
Statement: Innovaccer rolled out Flow Auth, an AI-powered prior authorization solution. Shashank told Fierce Healthcare at HIMSS26: “Prior auths, referrals, coding, denial management and scribing, all of these products are combined into one stack that we are calling the autonomous healthcare stack.”
With Innovaccer’s prior authorization solution, healthcare organizations are reporting significant reductions in clinician time spent on prior authorizations, from minutes down to seconds.
Infinx
Website: www.infinx.com
Contact Name: Jaideep Tandon, CEO
Statement: Infinx was named as a Representative Vendor in the Gartner 2026 Market Guide for Intelligent Prior Authorization on March 31, 2026. Jaideep Tandon said: “We believe our inclusion in the Gartner Market Guide reflects the growing need for intelligent automation in prior authorization workflows. Healthcare organizations are looking for scalable solutions that combine advanced technology with operational expertise to help manage complexity and support financial performance.”
UiPath
Website: www.uipath.com
Contact Name: Not specified (company press release)
Statement: At ViVE 2026 in February 2026, UiPath launched agentic AI solutions for healthcare providers and payers. The company said the offerings are designed to reduce administrative workload and payment delays, focusing on medical records summarization, claim denial prevention and resolution, and prior authorization.
Which Clinics and Hospitals Have Adopted This Strategy?
Here are real healthcare organizations across the United States that have implemented prior authorization automation, with links to their official websites.
Massachusetts
| Organization | What They Did | Link |
|---|---|---|
| Mass General Brigham | Used UiPath agentic AI for medical records summarization and prior authorization automation | www.massgeneralbrigham.org |
| Boston Children’s Hospital | Early adopter of AI-powered prior authorization workflows | www.childrenshospital.org |
Minnesota
| Organization | What They Did | Link |
|---|---|---|
| Mayo Clinic | Early user of UiPath agentic AI, reporting successful results in prior authorization automation | www.mayoclinic.org |
California
| Organization | What They Did | Link |
|---|---|---|
| Altais (formerly Brown & Toland Physicians) | Deployed Autonomize AI prior authorization application, cutting review time by 45% and manual errors by 54% | www.altais.com |
| Stanford Health Care | Implemented R1 prior authorization automation for faster approvals | www.stanfordhealthcare.org |
| UC Health | Uses RPA and automation for patient scheduling and prior authorization | www.uchealth.com |
Florida
| Organization | What They Did | Link |
|---|---|---|
| AdventHealth | Built custom RPA robots with UiPath and Automation Anywhere for prior authorization | www.adventhealth.com |
| Florida health system (name not disclosed) | Partnered with R1, achieving 99% prior authorizations cleared within three days | N/A |
Texas
| Organization | What They Did | Link |
|---|---|---|
| Memorial Hermann | Uses RPA for patient billing and prior authorization | www.memorialhermann.org |
| Houston Methodist | Implemented AI-powered prior authorization solutions | www.houstonmethodist.org |
Washington
| Organization | What They Did | Link |
|---|---|---|
| Providence Health | Uses RPA to manage billing and prior authorization across many hospitals | www.providence.org |
Pennsylvania
| Organization | What They Did | Link |
|---|---|---|
| Allegheny Health Network | Achieved “first-touchless prior authorization” using Humata Health (now part of Optum Digital Auth Complete) with 96% first-pass approval rate | www.ahn.org |
Michigan
| Organization | What They Did | Link |
|---|---|---|
| Trinity Health | Uses RPA to handle entire revenue cycle from start to finish | www.trinity-health.org |
National / Multi-State
| Organization | What They Did | Link |
|---|---|---|
| Kaiser Permanente | Uses RPA to fix denied claims automatically. RPA robots read denials, find missing information, and resubmit in minutes | www.kaiserpermanente.org |
| Allina Health (Minnesota, Wisconsin) | One of the first to deploy Optum Digital Auth Complete | www.allinahealth.org |
How a Fresh Clinic Can Automate Prior Authorization
If you run a small or medium clinic and want to start automating prior authorization, here is a simple 5-step plan.
| Step | What To Do | Time Needed |
|---|---|---|
| Step 1 | Pick one insurance payer that causes the most delays. Start small. | 1 week |
| Step 2 | Choose an automation tool. UiPath is good for beginners. R1 RCM and Optum are great for larger clinics. | 2 weeks |
| Step 3 | Connect the tool to your EHR (electronic health record system). Most tools offer easy integration. | 1-2 weeks |
| Step 4 | Run a pilot for 30 days. Let the AI suggest approvals while your staff checks the work. Measure time saved. | 30 days |
| Step 5 | Expand to more payers and more approval types. Track your denial rate and turnaround time. | Ongoing |
Pro Tip: Start with eligibility verification. It is the easiest and gives you quick wins. Then move to prior authorization for your most common procedures or medications.
Key External Resources
| Organization | What You Will Find | Link |
|---|---|---|
| CMS | Prior Authorization API requirements and final rule details | Visit CMS Page |
| R1 RCM | Prior authorization case studies and product info | Visit R1 RCM |
| Optum | Digital Auth Complete and InterQual Auth Accelerator | Visit Optum |
| ZeOmega | Smart Auth Optimizer AI-driven prior authorization | Visit ZeOmega |
| Innovaccer | Flow Auth AI-powered prior authorization | Visit Innovaccer |
| Infinx | Patient Access Plus prior authorization platform | Visit Infinx |
| UiPath | Agentic AI for healthcare prior authorization | Visit UiPath Healthcare |
| Gartner | 2026 Market Guide for Intelligent Prior Authorization | Visit Gartner |
Final Thoughts
Prior authorization does not have to be a nightmare. The new 2026 CMS rules give you leverage. AI tools give you speed. And hospitals like Mayo Clinic, Mass General Brigham, and Allegheny Health Network prove it works.
You can save your staff thousands of hours. You can get patients their medicine faster. You can reduce denial rates to nearly zero.
The best time to start automating prior authorization was last year. The next best time is today.
If you need prior authorization automation for your clinic or hospital, Cureintent is here to help you. We help healthcare organizations just like yours simplify prior authorization and revenue cycle management using smart technology and easy-to-understand guidance. Visit Cureintent.com to learn more about how we can help your clinic automate prior authorization, reduce denials, and get paid faster.
“Automate Prior Auth, Accelerate Care, Partner with Cureintent”