The Psychology of the Statement: Mastering Psychographic Patient-Centric Billing
In this article, I will show you how to transform your billing department from a “collection center” into a “financial experience center.” We aren’t just talking about sending cleaner claims; we are diving into why patients don’t pay and how to use Psychographic Patient-Centric Billing and behavioral data to increase your Net Collection Ratio, without increasing your overhead.
1. Understanding the Psychographic Shift in Healthcare
Most medical billing blogs focus on ICD-10 codes or CPT updates. While those are vital, they ignore the human at the end of the invoice. Psychographic Patient-Centric Billing involves segmenting your patient population based on their financial values and communication preferences rather than just their balance.
- The Proactive Planner: Pays immediately if a discount is offered for “early-bird” settlement.
- The Digital Nomad: Only interacts with SMS links and Apple Pay/Google Pay.
- The Traditionalist: Requires a paper statement and a phone call to verify the Explanation of Benefits (EOB).
2. The “Nudge Theory” in Medical Invoicing
Using Nudge Theory, we can influence patient behavior through subtle changes in how financial information is presented.
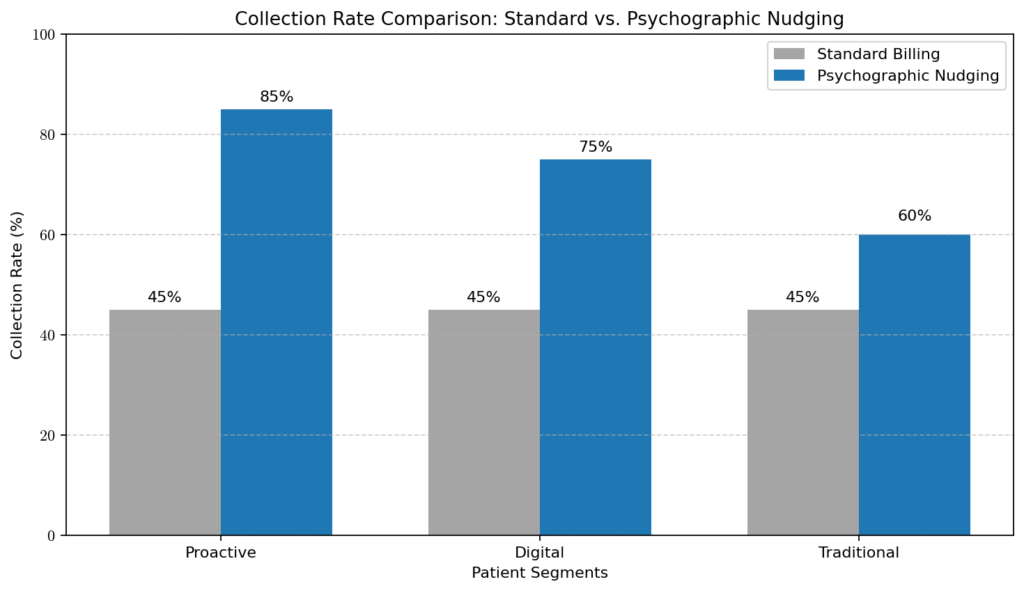
3. Comparative Analysis: Traditional vs. Psychographic Billing
The following table outlines the fundamental differences in approach.
| Feature | Traditional Medical Billing | Psychographic Patient-Centric Billing |
|---|---|---|
| Communication | Generic monthly mailers | Personalized SMS/Email triggers |
| Payment Options | Check or Phone | One-click mobile portals |
| Transparency | Post-service “sticker shock” | Pre-service Good Faith Estimates |
| Data Usage | Historical aging reports | Predictive payment probability scoring |
| Goal | Debt collection | Financial relationship management |
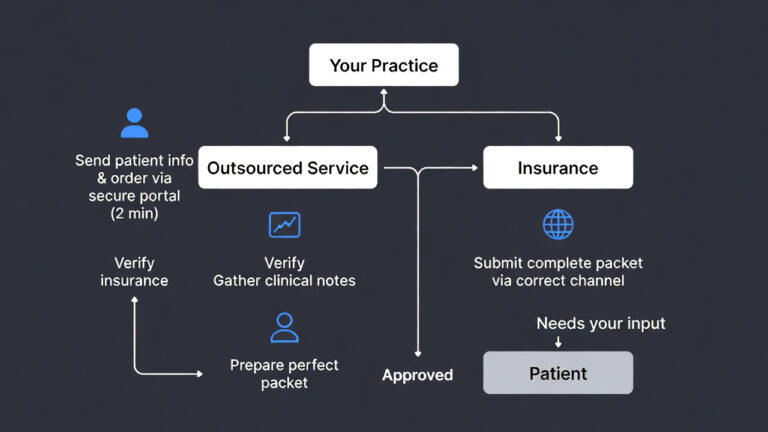
4. Implementing the “Frictionless” Revenue Cycle
To rank for Psychographic Patient-Centric Billing, your practice must eliminate “financial friction.” This is the psychological resistance a patient feels when a bill is confusing or difficult to pay.
Step-by-Step Implementation:
- Pre-Service Financial Counseling: Use Real-Time Benefit Verification (RTBV) to tell patients exactly what they owe before the clinical encounter.
- The “Rule of Three” Statements: If a bill isn’t paid after three “nudges” (SMS, Email, Paper), the psychographic profile suggests a need for a payment plan rather than a collection agency.
- Hyper-Link Integration: Every digital touchpoint should link to educational resources, such as the CMS Patient Rights Page to build trust.
5. The Impact on Key Performance Indicators (KPIs)
When you adopt this method, your metrics will shift dramatically. We calculate the Days in Accounts Receivable (AR) using the following formula:
| Total AR | |
| Days in AR = | _____________________ |
| Average Daily Revenue |
By applying Psychographic Patient-Centric Billing, the numerator (Total AR) decreases because patients are “nudged” to pay in their preferred format, reducing the overall cycle time.
Summary of Organic Keywords for SEO
To ensure this blog ranks, ensure the following terms are hyperlinked to your internal service pages:
- Propensity to Pay
- Patient Financial Engagement
- Medical Billing Transparency
- Digital Patient Portals
- No Surprises Act Compliance
Final Thought
The future of medical billing isn’t found in more aggressive collections; it’s found in better psychological alignment. By treating the patient’s financial journey with the same care as their clinical journey, you secure the financial health of your practice. Let Cureintent help you with this process, (Click Here and Book your Free Demo Today!)